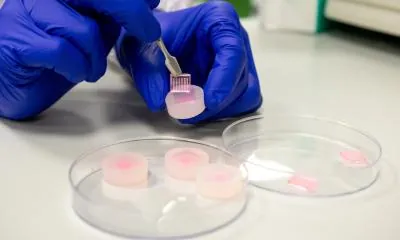
Revolutionary Microneedle Technology Boosts Healing for Diabetic Wounds – A Game Changer for Patients!
2025-03-31
Author: Jia
Introduction
As diabetes continues to pose severe health risks globally, recent innovations in wound care could spell hope for many. In Singapore alone, an alarming four lower limb amputations occur daily due to complications arising from non-healing diabetic wounds, amassing healthcare costs as substantial as S$23,000 per patient just in 2017.
Microneedle Technologies Developed
To combat this pressing issue, a team of researchers from the National University of Singapore (NUS) has engineered two groundbreaking microneedle technologies that promise to accelerate the healing process for diabetic wounds. These advancements focus on preserving the activity of vital proteins called growth factors while simultaneously removing harmful inflammatory compounds. This minimally invasive method ensures effective treatment while reducing patient discomfort.
Research Team
Led by Assistant Professor Andy Tay, from the Department of Biomedical Engineering, this innovative team has unveiled microneedle patches that are not only precise but also painlessly deliver therapeutic agents directly into wounds. “Growth factors play a critical role in the healing process, but their effectiveness is often compromised by proteases, which break them down too quickly in diabetic wounds. Our goal was to tackle both the decay of these factors and the chronic inflammation typical of diabetic injuries,” explained Tay.
Applications and Studies
The studies documenting these advancements have been published in renowned scientific journals, underscoring the potential applications of microneedle technology for various skin conditions, including psoriasis and chronic wounds associated with diabetes.
First Approach: Sucralfate Microneedles (SUC-MN)
In a first approach, the NUS team developed sucralfate microneedles (SUC-MN) designed to enhance growth factor production within the wound. By delivering interleukin-4 (IL-4), an immunomodulatory protein that stimulates growth factor synthesis, these microneedles effectively catalyze tissue regeneration. The dual action of SUC-MN provides localized delivery that minimizes systemic side effects, significantly accelerating healing times — observed to be twice as fast compared to standard treatments.
Second Approach: Heparin-coated Porous Microneedles (HPMN)
The second strategy, using heparin-coated porous microneedles (HPMN), innovatively targets the removal of inflammatory proteins and immune cells, which often hinder the healing process. By acting like a sponge, these microneedles can effectively reduce tissue inflammation by 50% and decrease wound size by 90% within just two weeks of treatment, showing a promising avenue for managing inflammatory skin disorders more efficiently than traditional methods.
Future Enhancements
Looking ahead, the team aims to enhance their microneedle designs by employing advanced technologies like 3D printing to provide customizable pore sizes and incorporate antibacterial properties to combat potential infections in non-healing wounds.
Conclusion
Asst Prof. Tay expressed enthusiasm about the impact of this research: "We are excited about our findings and are committed to advancing this technology toward clinical use. This innovation could be transformative for patients with diabetic wounds and numerous skin conditions, markedly improving their quality of life." Stay tuned as these revolutionary microneedle technologies pave the way for a new era in diabetic wound care and skin disease management!



 Brasil (PT)
Brasil (PT)
 Canada (EN)
Canada (EN)
 Chile (ES)
Chile (ES)
 Česko (CS)
Česko (CS)
 대한민국 (KO)
대한민국 (KO)
 España (ES)
España (ES)
 France (FR)
France (FR)
 Hong Kong (EN)
Hong Kong (EN)
 Italia (IT)
Italia (IT)
 日本 (JA)
日本 (JA)
 Magyarország (HU)
Magyarország (HU)
 Norge (NO)
Norge (NO)
 Polska (PL)
Polska (PL)
 Schweiz (DE)
Schweiz (DE)
 Singapore (EN)
Singapore (EN)
 Sverige (SV)
Sverige (SV)
 Suomi (FI)
Suomi (FI)
 Türkiye (TR)
Türkiye (TR)
 الإمارات العربية المتحدة (AR)
الإمارات العربية المتحدة (AR)