Unraveling the Hidden Link: How Depression Amplifies Cardiovascular Risks in Cancer Patients
2025-03-31
Author: William
In an alarming revelation, recent research highlights a dangerous intersection between two of the leading causes of global mortality: cardiovascular disease (CVD) and cancer. With cardiovascular disease responsible for a staggering 32% of deaths worldwide in 2019 and cancer contributing to 16.8%, understanding their relationship has profound implications for public health.
A complex web of factors uniquely positions cancer patients at greater risk for both conditions. Chronic inflammation and oxidative stress, fueled by shared genetic vulnerabilities, create a biological bridge linking CVD and cancer that complicates treatment. Not only do cancer therapies risk accelerating atherosclerosis, but pre-existing cardiovascular conditions can also hinder effective cancer management. This overlap creates formidable clinical challenges that must be addressed.
As the prevalence of cardiovascular disease escalates, particularly among older populations battling diabetes, hypertension, and obesity, the damaging effects of cancer therapies come into sharper focus. Chemotherapeutic agents, particularly anthracyclines, can lead to cardiomyopathy through mitochondrial dysfunction, while radiation therapy poses additional risks by damaging blood vessels—key contributors to coronary artery disease.
Adding psychological stressors into this melting pot, studies reveal that between 15% to 25% of cancer patients experience depression, exacerbating cardiovascular risk through neurohormonal activation and chronic inflammation. This bidirectional relationship emphasizes the urgent need for an integrated approach to treatment known as cardio-oncology—an emerging field dedicated to understanding and mitigating cardiovascular risks for cancer patients.
One of the novel assessment tools being utilized is the Cardiometabolic Index (CMI), which is particularly relevant for cancer survivors. This metric accounts for cardiovascular risks stemming from both psychological factors like depression and physiological vulnerabilities, helping healthcare providers deliver tailored interventions that can improve patient outcomes.
The interplay of depression and cardiovascular health becomes even more critical as survival rates for cancer improve. Longitudinal studies are increasingly revealing surprising statistics: cardiovascular mortality rates among breast and prostate cancer survivors now outpace cancer-specific mortality after ten years. This alarming trend underscores the vital need for early identification and management of depression in this high-risk population.
A retrospective cohort study uncovered a shocking statistic: the treatment of depression with selective serotonin reuptake inhibitors (SSRIs) led to a 38% reduction in heart failure incidences among lymphoma survivors. The integration of mental health treatment into standard cancer care could lead to significant improvements in cardiovascular health outcomes.
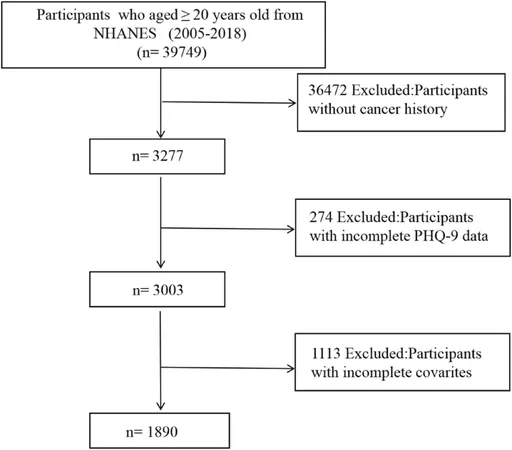
While the connection between depression and CVD is well recognized in the general population, the cardiotoxic environment created by cancer treatments may intensify this relationship through shared physiological pathways. As ongoing research analyzes this dynamic using data from the National Health and Nutrition Examination Survey (NHANES), the goal is clear: to reshape clinical guidelines and healthcare practices that address both mental health and cardiovascular risks for cancer patients effectively.
The startling findings from the NHANES data pertain to 1,890 cancer patients, highlighting the complex vulnerability of those overlapping with mental health struggles. In this cohort, higher levels of depressive symptoms were directly associated with increased cardiovascular risks. As researchers delve deeper into these correlations, the evidence will inform policy changes aimed at advocating for routine depression screenings and tailored interventions.
Cancer patients are not merely battling their illness; they are navigating a minefield of psychological and physiological risks that can drastically affect their overall quality of life. Recognizing this intersection is not just a matter of academic interest but a critical step toward implementing comprehensive care models that address the needs of this unique population.
In the race to improve cancer care, addressing the mental health of patients may hold the key to better heart health, ultimately saving lives and improving the longevity of survivors. What does this mean for the future of cancer treatment? As studies continue to unveil these interconnected health risks, the adoption of an integrated approach could revolutionize care for millions of patients worldwide, potentially lowering cardiovascular incidence and mortality rates among cancer survivors.
Stay tuned as we uncover more about this crucial health nexus and advocate for necessary changes in healthcare practices!








 Brasil (PT)
Brasil (PT)
 Canada (EN)
Canada (EN)
 Chile (ES)
Chile (ES)
 Česko (CS)
Česko (CS)
 대한민국 (KO)
대한민국 (KO)
 España (ES)
España (ES)
 France (FR)
France (FR)
 Hong Kong (EN)
Hong Kong (EN)
 Italia (IT)
Italia (IT)
 日本 (JA)
日本 (JA)
 Magyarország (HU)
Magyarország (HU)
 Norge (NO)
Norge (NO)
 Polska (PL)
Polska (PL)
 Schweiz (DE)
Schweiz (DE)
 Singapore (EN)
Singapore (EN)
 Sverige (SV)
Sverige (SV)
 Suomi (FI)
Suomi (FI)
 Türkiye (TR)
Türkiye (TR)
 الإمارات العربية المتحدة (AR)
الإمارات العربية المتحدة (AR)